Can Botox Really Relieve Jaw Pain and Teeth Grinding?
← Back to Blog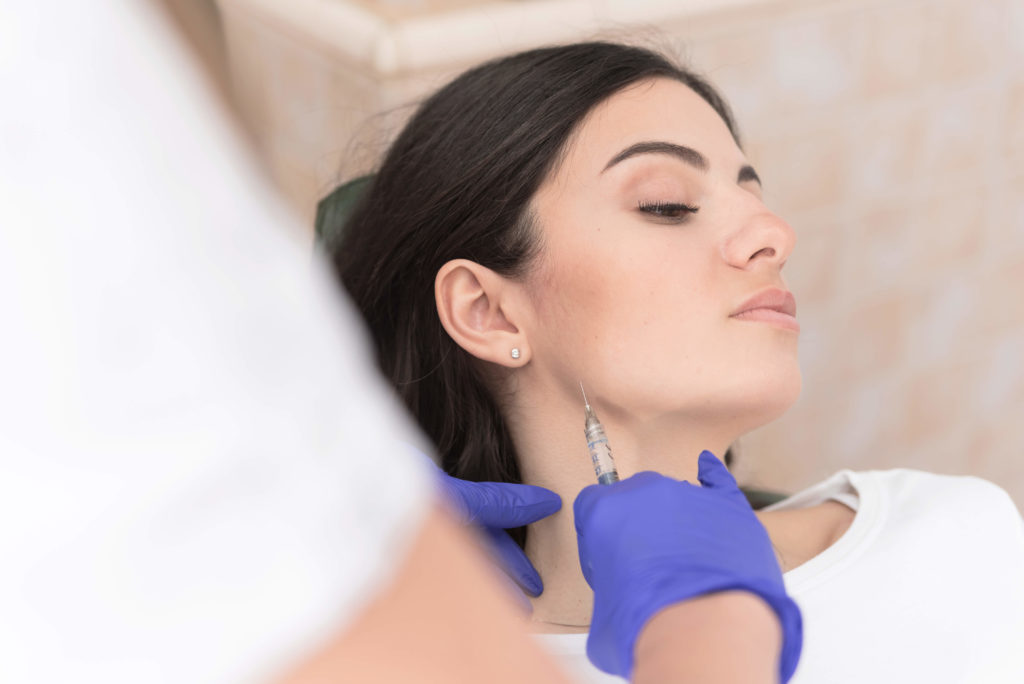

Chronic jaw pain, clicking joints, morning headaches and worn-down teeth — these are the hallmarks of TMJ disorder and bruxism (teeth grinding). They affect an estimated 10–15% of adults, and for many, finding effective relief is a years-long frustration. Botox has emerged as one of the most effective interventions available — and it's an area where BotoxYYC's dental background gives us a genuine clinical edge.
The masseter is the powerful chewing muscle at the angle of the jaw. In patients with TMJ disorder or bruxism, this muscle is chronically overactive — contracting with far more force than chewing food requires. The result is muscle fatigue, joint inflammation, referred headaches and, over time, significant wear on the teeth. Stress is a major contributing factor, but bite mechanics, sleep posture and genetics also play a role.
Injecting botulinum toxin directly into the masseter muscle temporarily reduces its contractile strength. The muscle is still functional for chewing — we dose conservatively to ensure this — but the excessive, damaging clenching force is significantly reduced. Most patients notice pain relief within 1–2 weeks, with full effect at 4–6 weeks as the muscle gradually reduces in activity.
A secondary effect that many patients appreciate: as the masseter reduces in size over time with repeat treatments, the lower face softens and narrows, creating a more oval, feminine jawline contour.
This is worth emphasising. Dentists and dental professionals study the anatomy of the jaw, temporomandibular joint, surrounding musculature, bite mechanics and occlusion (how teeth come together) in far greater depth than a general aesthetics provider. We understand the functional relationship between jaw muscles, the joint and the teeth — which means our assessment of TMJ cases is genuinely clinical, not just cosmetic.
We can assess whether your symptoms are likely to respond well to masseter Botox, identify contributing dental factors, and integrate treatment with any other dental care you may need. This is a level of comprehensive management most aesthetics clinics simply can't provide.
Treatment is straightforward: a series of injections into the belly of the masseter muscle on each side of the face, using a very fine needle. Most patients require 25–50 units per side depending on muscle mass. The procedure takes approximately 15 minutes with no downtime. We recommend avoiding hard, chewy foods for two weeks following treatment to allow the muscle to settle.
Initial results typically last 3–6 months. With repeat treatments at consistent intervals, many patients find the duration extends — likely because the reduced muscle activity leads to genuine muscle atrophy over time, meaning less product is needed to maintain the effect. Some patients who have been treated consistently for 1–2 years find they can stretch intervals to 6–8 months.
Masseter Botox is appropriate for most healthy adults with TMJ symptoms, jaw pain or bruxism. It is not suitable during pregnancy, for patients with neuromuscular conditions, or for those with active infection at the injection site. A consultation allows us to assess your individual situation and advise whether it's the right approach for you.